The HPV4 vaccine, Gardasil, is safe for adolescent girls and young women in routine clinical care, researchers from the Kaiser Permanente Vaccine Study Center in Oakland, California, reported in Archives of Pediatrics and Adolescent Medicine.
The vaccine is linked to a slight risk of same-day fainting (syncope) as well as skin infections within two weeks. The researchers said that their findings provide further compelling evidence of the HPV4’s general safety for routine use in a clinical care setting for the prevention of cervical cancer as well as other reproductive and genital cancers.
The authors said that the link between fainting and the vaccine was not a surprise, because injections can sometimes have that effect on people, especially younger patients. As far as the risk of infection was concerned, indications suggest that they were mostly cases of injection-site reactions – however, there was not enough data to be able to rule out acute infections. A number of females sought increased clinical care for skin conditions following vaccinations.
Lead author Nicola Klein, MD, PhD, said:
“Taking into account all the analyses, subanalyses and relevant medical record reviews, an independent safety committee noted that there may be an association between HPV4 vaccination and same-day syncope, as well as skin infections during the two weeks after immunization.”
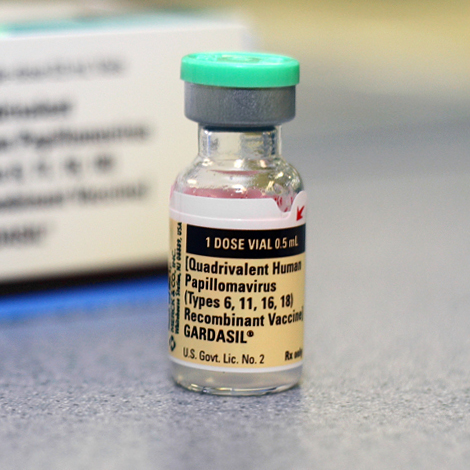
Gardasil vaccine – HPV4 (quadrivalent human papillomavirus vaccine)
Quadrivalent means it is valid against four HPV types – HPV 16 and 18 which cause cancers, and HPV 6 and 11 which cause genital warts.
HPV (human papillomavirus) is a family of tiny DNA viruses that affects human skin and the moist membranes that line the body, such as the throat, mouth, feet, fingers, nails, anus and cervix.
There are more than 100 types of HPVs, of which 40 may affect the genital area. The HPV 16 and 18 strains are known to cause nearly all cases of cervical cancer
HPV infections are the most commonly sexually transmitted infections in females. In the majority of cases, infected women experience no symptoms and it resolves on its own.
Persistent genital HPV infection can lead to cervical cancer in females, as well as cancers of the penis, vagina, anus and oropharynx (oral part of the pharynx – throat cancer). HPVs can also cause genital warts in males and females.
The quadivalent HPV vaccine, or HPV4 was approved by the Food and Drug Administration (FDA) for females aged from 9 to 26 years for the prevention of HPV infections and the diseases it can cause.
Dr. Klein and team carried out a retrospective, observational study of all the girls and women who were given the HPV4 vaccine at Kaiser Permanent in California. The study was funded by Merck & Co, the manufacturers of the vaccine, Gardasil. In an online communiqué, JAMA wrote “The study was a postlicensure commitment to the Food and Drug Administration and the European Medicines Agency after initial licensure in females.”
The authors concluded:
“In summary, this study of 189,629 females who received HPV4 found that immunization was associated with same-day syncope and skin infections in the two weeks after vaccination. The findings from this large, comprehensive study did not detect any evidence of serious safety concerns secondary to HPV4. These findings support the general safety of routine vaccination with HPV4 to prevent cancer.”
The researchers compared the risk of emergency department visits among the vaccinated females, as well as hospitalization soon after being vaccinated, and then again a longer time after vaccination. The patients received at least one dose of HPV4 vaccine between August 2006 and March 2008. The group received a total of 346,972 HPV4 doses.
An independent Safety Review Committee reported only skin infections from day 1 to 14 with an odds ratio of 1.8 and syncope (fainting) on the vaccination day with an odds ratio of 6.0 as likely adverse events linked to HPV4.
According to the Centers for Disease Control and Prevention, patients should be monitored for 15 minutes after receiving the vaccine (in case they faint). Gardasil’s prescribing information recommends the same.
Only two HPV vaccines have been approved in the USA – Merck’s Gardasil and GlaxoSmithKline’s Cervarix. Cervarix earned the company $812 million last year, compared to Gardasil’s $1.2 billion.
Written by Christian Nordqvist