Adding antibiotics to livestock feed should be banned, the Ontario Medical Association (OMA) urged today. In a report titled “When Antibiotics Stop Working”, the authors are also calling for stricter guidelines regarding the human use of antibiotics.
The report explained that doctors are facing the extinction of one of the most fundamental and life-saving tools in medicine – effective antibiotics. Doctors in Ontario, and the rest of the world too, are calling on their governments to take the growing problem of antibiotic resistance seriously while there is still time.
Infections with antibiotic-resistant bacteria are becoming more and more common, says the Ontario Medical Association. These infections are difficult to treat; patients have a serious risk of becoming extremely ill and even dying.
The over-use of antibiotics undermines their ability to save human lives. OMA calls on Canada’s federal and provincial governments to put in place legislation so that the growing problem of antibiotic resistance may be reversed.
Bacteria are adapting to our antibiotics – they are not as effective as they used to be. These bacteria can cause skin infections, urinary tract infections, and pneumonia.
A decade ago, a child suffering from strep throat could be treated effectively with just one dose of antibiotics. Today this is becoming less likely. Children are having repeated strep throat infections, which commonly have complications, such as scarlet fever.
If the first choice of antibiotics is not effective, the doctor has to prescribe newer and stronger ones with more severe side effects.
People who have access to antibiotics need to start using them as prudently as possible, the authors wrote. This includes closing the loophole that allows farmers to add antibiotics to their livestock feed, to promote growth, without requiring a prescription. It also means that patients’ antibiotic histories need to be tracked more thoroughly so that the right medications may be prescribed.
The report recommends:
- Set up a system whereby we know who is buying antibiotics in the farming industry, and how much is being bought. Also, within this system, include data on antibiotic movement in or out of Ontario.
There is currently no surveillance of antibiotic movement in Ontario.
- Set up an independent body to develop and maintain best antibiotic use guidelines that Ontario doctors can use to guide their practice, especially when confronted with resistant bacteria and less familiar antibiotics.
- Institute a veterinary prescription-only standard of antibiotic access for livestock
- Close the loophole which allows farmers to import antibiotics for own use, and amend the Food and Drugs Act
Dr. Doug Weir President Ontario Medical Association, said:
“Ontario’s doctors are concerned about the growing rate of antibiotic resistant bacteria. Patients are at risk of becoming sicker, taking longer to recover and it some cases dying from previously treatable diseases. Data shows that we can reduce antibiotic resistant bacteria when the use of antibiotics is modified. Adopting the recommendations in the report will help us achieve this.”
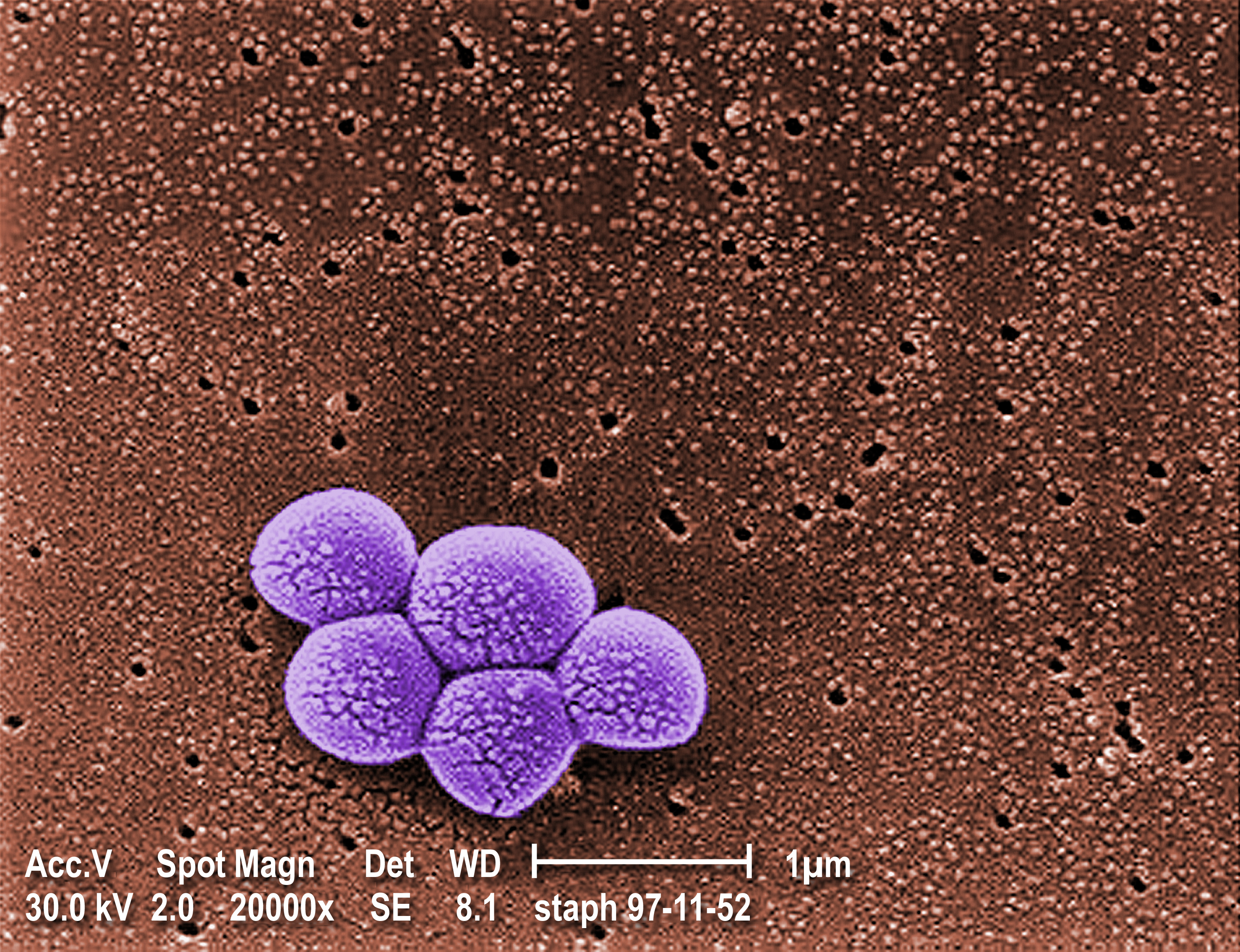
Electron micrograph of methicillin resistant Staphylococcus aureus (MRSA) bacteria, magnified 20,000x
- In 1977, the US FDA concluded that adding antibiotics for human medicine to livestock feed raised the risk of antibiotic-resistant bacteria. Peter Lehner, from the Natural Resources Defense Council (NRDC) asked why nothing has been done over the last 35 years.
Peter Lehner said:
“More than a generation has passed since FDA first recognized the potential human health consequences of feeding large quantities of antibiotics to healthy animals.
Accumulating evidence shows that antibiotics are becoming less effective, while our grocery store meat is increasingly laden with drug-resistant bacteria. The FDA needs to put the American people first by ensuring that antibiotics continue to serve their primary purpose – saving human lives by combating disease.”
Seventy percent of all antibiotic consumption in the USA is used up by the farming industry – most of it used by adding it to livestock feed. The main reason is to promote faster growth and reduce disease, especially when animals are in unsanitary living conditions, says the NRDC.
- England’s Chief Medical Office, Dame Sally Davies, in March 2013, warned that within the next two decades people may die after simple operations because of antibiotic resistance – there may be no antibiotics left to deal with routine infections.
She said that antibiotic resistance should now be added to the UK government’s list of civil emergencies.
- The European Centre for Disease Prevention and Control (ECDC) declared in November 2012 that antibiotic resistance has become a major threat to public health worldwide. For the large part, it has been caused by antibiotic misuse.
The ECDC said that antibiotic resistance:
– Raises healthcare costs
– Increases lengths of hospital stays
– Causes more treatment failures
– Results in more human deathsApproximately 25,000 patients die annually in the European Union from infections caused by antibiotic-resistant bacteria.
Combined resistance to multiple antibiotics has been found in E. coli and Klebsiella pneumonia in various parts of Europe.
Written by Joseph Nordqvist