A Pap smear is a screening tool that healthcare professionals use detect abnormal cells and cancer. During the Pap smear, a healthcare professional takes a cell sample from the cervix.
Cervical cancer is a type of cancer that develops in the cells in the lower part of the uterus. This region is called the cervix, it is small and narrow, and it connects the uterus to the vagina. It provides an entry for sperm to pass into the uterus. The cervix also provides an exit from the uterus for monthly menstrual blood flow or a baby during delivery.
There are two parts to the cervix, and two different types of cells occur there:
Endocervix: This is the innermost part of the cervix. It lines the “tunnel” leading from the uterus into the vagina. It contains tall, column-like cells that are responsible for mucus secretion.
Ectocervix: This is the outer portion of the cervix, and it protrudes into the vagina. The ectocervix is home to squamous cells, which resemble fish scales under the microscope.
Where these two cell types meet is where
A Pap smear is a screening tool that can help doctors detect abnormal cells and cancer. It works by sampling cells from the cervix.
Cervical cancer screening is vital for getting an early diagnosis of cervical cancer. With an early diagnosis, effective treatment is usually possible.
Doctors recommend two tests for this purpose:
- The Pap smear, which checks for abnormal cells.
- The human papillomavirus (HPV) test, which detects DNA from HPV to reveal both its presence and type.
This information can help a doctor determine whether a person has cervical cancer, or if they have an increased risk of developing this disease.
These tests can detect:
- precancerous cell changes
- the presence of HPV
- the presence of cancer
If the tests lead to a diagnosis, a person can then seek treatment.
Routine screening does not always automatically include both tests at the same time, but a person can ask for an HPV test at the same time as a Pap smear.
According to the American Cancer Society (ACS), deaths from cervical cancer
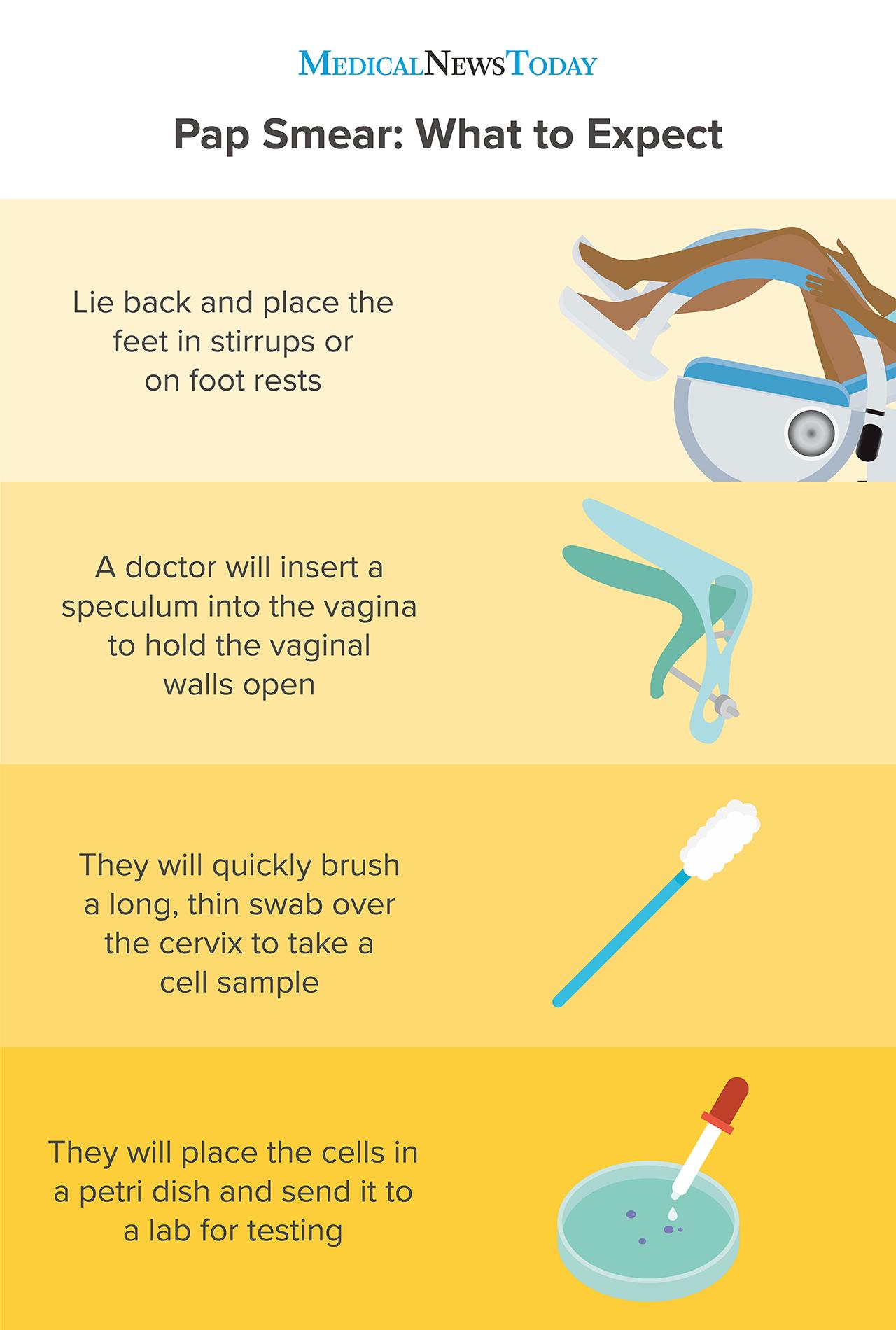
A doctor usually carries out a Pap smear during a gynecological pelvic exam. They insert a tool called a speculum into the vagina so that they can examine the cervix. Then, they take a sample of cervical cells using a brush or spatula and send them for testing.
If possible, it is best to avoid having a Pap smear during a menstrual period, especially if the flow is heavy, as this can affect the results of the test. However, if a person only has the chance to have the test during menstruation, it is still better to attend than not.
A person should not douche or put anything in the vagina to clean it before the test. Doctors do not recommend douching at any time.
Recommendations on Pap smear frequency depend on several factors.
These include:
- age
- medical history
- exposure to diethylstilbestrol (DES) when in the womb
- HIV status
- whether or not the person has a weakened immune system, for example, due to HIV
The
- Women aged 21–29 years should have a Pap test every 3 years.
- Women aged 30–65 years should have a Pap test every 3 years, or an HPV test every 5 years, or a Pap and HPV co-test every 5 years.
The American Cancer Society
After the age of 65 years, most women will not need a Pap smear or HPV test. However, each person’s risk factors vary.
Those who have had abnormal test results in the past and those who are sexually active with more than one partner may need more frequent testing.
After a total hysterectomy, which is the surgical removal of the uterus and cervix, a Pap smear will no longer be necessary.
Anyone who has a hysterectomy because they had cancerous or precancerous cells should continue to have regular tests.
Everyone has different needs, so it is important that people speak to their doctor about their risk factors for developing cervical cancer and their need for screening.
The test results usually take 1–3 weeks to come back. Most test results are negative, but they can sometimes be positive. A positive result does not confirm that a person has cancer, but it indicates that more investigation is necessary.
Normal
In most Pap smears, the result is normal and does not reveal any abnormal cells.
Unclear
Sometimes the result is ambiguous. The doctor may ask the person to have more tests to monitor for any changes. These additional tests are likely to take place either soon after the first test or about 6 months later.
Abnormal
Sometimes the result is “abnormal.” The doctor may recommend more tests straight away or after 6 months depending on the extent of the cell changes.
Common cell abnormalities include:
Atypical squamous cells of undetermined significance (ASCUS): These are mildly abnormal cells that do not meet the criteria for precancerous cells. If HPV is present, the doctor may recommend additional testing.
Squamous intraepithelial lesion: These lesions indicate possible precancerous cellular changes that are likely to need further testing.
A doctor will usually recommend following up with a colposcopy, with or without a biopsy.
During a colposcopy, the doctor uses a colposcope to magnify the view of the cervix, vulva, and vagina for examination. They may take a biopsy sample for evaluation in a laboratory.
They are divided into two categories:
- Low grade: A low-grade lesion has a low risk of progressing to cancer in the near future.
- High grade: A high-grade lesion has a high risk of progressing to cancer sooner rather than later.
- Atypical glandular cells: This diagnosis is indicative of abnormal cells in the endocervix. These will require further testing.
- Squamous cell cancer or adenocarcinoma: This diagnosis signals the likelihood of cancer and depends on the cell type that is atypical. Further testing is required.
What does an abnormal result mean?
It is possible to classify the cell changes as follows:
Low-grade lesion: The risk of a low-grade lesion imminently progressing to cancer is minimal.
High-grade lesion: A high-grade lesion has a high likelihood of becoming cancerous sooner rather than later.
Atypical glandular cells: There are abnormal cells in the endocervix that will need further testing.
Squamous cell cancer or adenocarcinoma: There is a likelihood of cancer, depending on the type of cell that is atypical. Further testing is necessary.
In 2019, the ACS estimate that there will be
Screening and other types of prevention can reduce this risk dramatically.
There are often no symptoms until the later stages, when there
Risk factors for developing cervical cancer
- not having the HPV vaccine
- not attending routine screenings
- having an HPV infection
- smoking
- having sex without using a condom
- having several sexual partners
- having a chlamydia infection
- having a weakened immune system, for example, due to HIV
- not including enough fruit and vegetables in the diet
- being overweight
- using birth control pills for an extended period
- using an intrauterine device (IUD) for birth control
- having several full-term pregnancies
- being under 18 years of age for the first full-term pregnancy
- taking the hormonal drug DES or having a mother who used it
Doctors also do not recommend douching, as this can increase the likelihood of exposing the vagina to bacterial infection.
What is human papillomavirus?
HPV is a virus that can lead to cervical cancer in some cases. There are
Other types can lead to different complications, such as noncancerous warts or papillomas.
HPV can pass from one person to another during vaginal, anal, or oral sex when there is skin-to-skin contact.
There is no cure, but the infection often resolves in time. However, if HPV becomes a long-term infection, the risk of cancer increases.
Treatment is available for HPV-related warts and cell changes.
Vaccination is available to protect against HPV infection. Until recently, the Centers for Disease Control and Prevention (CDC) have recommended that young women have the vaccine up to the age of 26 years and young men up to 21 years.
In 2018, however, the
Cervical cancer is a type of cancer that develops in the cervix. Before developing into cancer, cervical cells undergo abnormal changes that a Pap test can detect.
With early diagnosis and appropriate treatment, the chances of surviving cervical cancer are good.
If a doctor diagnoses cervical cancer in its earliest stage, the person has
The
