Dry skin patches can have many causes, including cold weather and the chemicals in some soaps and lotions. It can also result from a medical condition, such as allergies, dermatitis, and psoriasis.
Dry skin is a common problem during the winter months when the skin is exposed to colder temperatures and lower moisture levels in the air. In these cases, moisturizer is often enough to soothe and eliminate dry skin patches.
However, some people experience chronic or long lasting, dry skin. This can indicate an underlying medical condition that would benefit from treatment.
This article describes some common medical conditions and other factors that can cause dry skin and how to deal with them.
The skin can become dry, scaly, or flaky for many reasons, such as exposure to chemicals in soaps or harsh, windy weather.
Other causes of dry skin include:
- using hot water
- excessive handwashing
- dehydration
- poor nutrition
- lotions that contain alcohol
In many cases, a person can alleviate dry skin by regularly applying moisturizer to the affected area and avoiding cleaning and personal care products containing harsh chemicals.
In some cases, however, dry skin patches require specific treatment.
Skin conditions can worsen in cold weather, including dermatitis, which broadly refers to any condition that causes skin inflammation. There are many types of dermatitis.
The following skin conditions can cause patches of dry skin:
Contact dermatitis
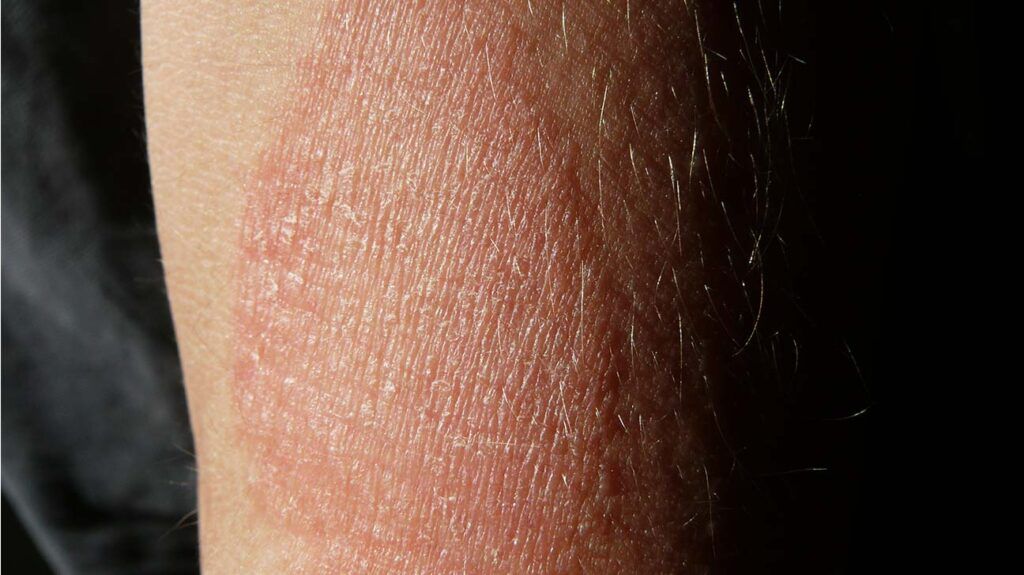
This type of dermatitis usually results from contact with an allergen, such as poison ivy or animal dander. Some laundry detergents can also trigger an allergic reaction.
People can prevent reactions by identifying and avoiding the trigger for the dermatitis.
Contact dermatitis occurs on the area of the skin that comes into contact with the allergen. It is common on exposed areas of skin, such as the hands and face.
Symptoms of contact dermatitis include:
- dry, scaly patches of skin
- hives
- an itching or burning sensation on the affected areas
- open or leaking blisters
Contact dermatitis can appear red or pink on lighter skin tones and dark brown, purple, or gray on darker skin.
Learn more about contact dermatitis.
Atopic dermatitis
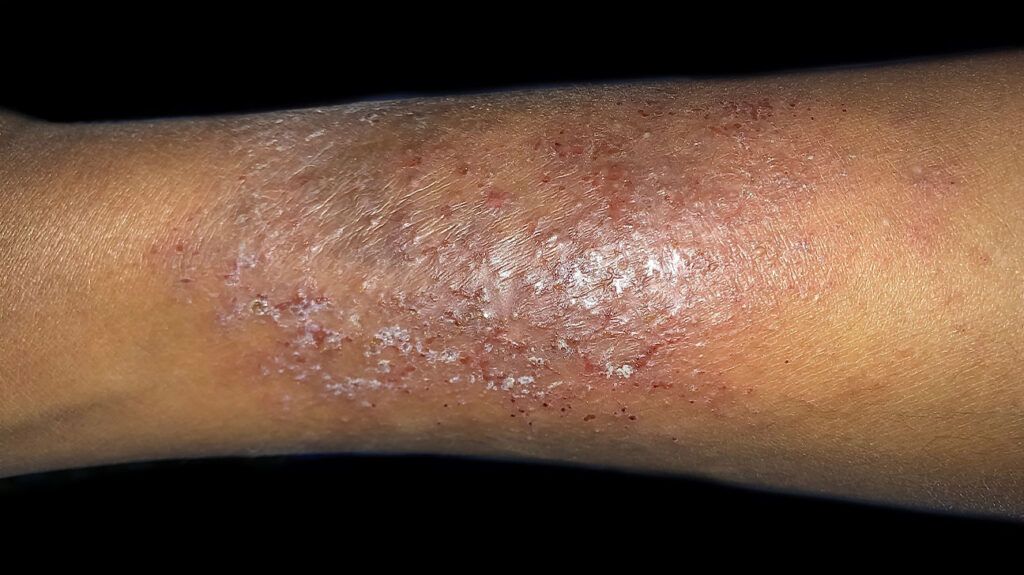
Atopic dermatitis, or eczema, is a chronic skin disease that
Atopic dermatitis can appear anywhere but, in adults and teens, it is common on the hands, neck, feet and ankles, around the eyes, and in elbow and knee creases.
Symptoms include:
- dry, irritated skin
- scaly skin
- a rash
- itchiness
- cracked skin behind the ears
On darker skin tones, atopic dermatitis can cause darker or lighter areas of inflamed skin. It may appear red or pink on lighter skin tones.
Learn more about atopic dermatitis.
Seborrheic dermatitis
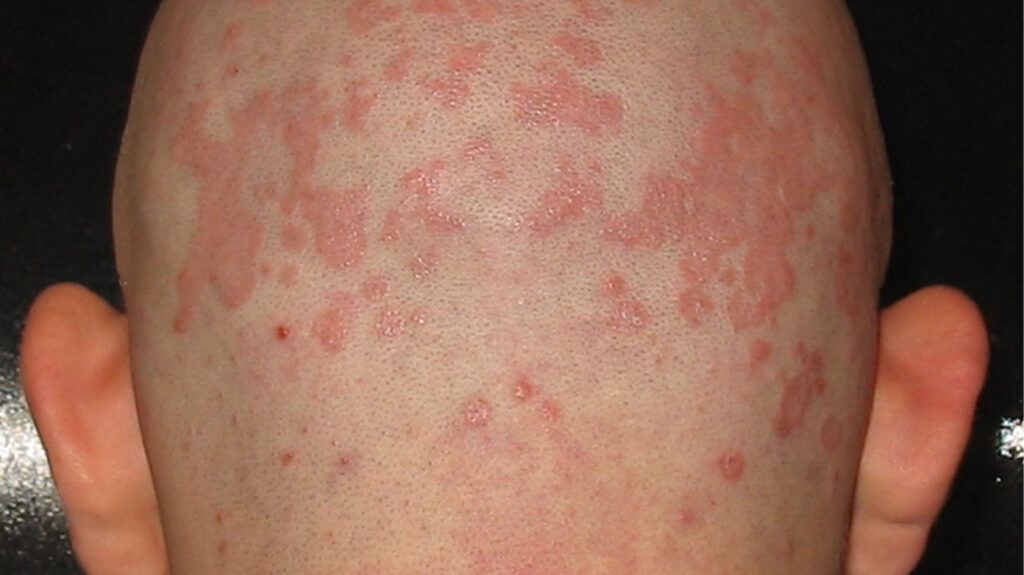
Seborrheic dermatitis is a skin condition that occurs when the sebaceous glands produce too much oil. It typically causes patches of white, crusty flakes on the scalp, face, chest, and back.
On darker skin tones, seborrheic dermatitis may cause scaly, lighter patches of skin in inflamed areas. Curved or petal-shaped patches may occur.
When the condition affects infants, it is called cradle cap.
Other symptoms of seborrheic dermatitis include:
- thin scales that are lighter than a person’s normal skin tone
- oily or greasy patches of skin
- red patches of skin
- itchiness
Learn more about seborrheic dermatitis.
Ichthyosis vulgaris
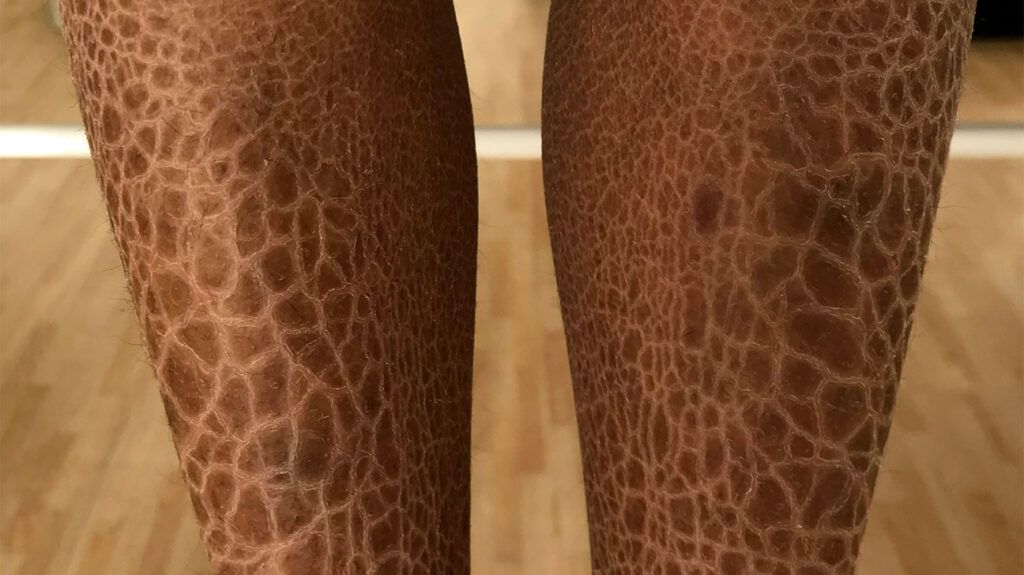
“Ichthyosis” is a term that refers to a group of genetic skin disorders that cause dry, scaly skin.
Most forms are extremely rare, and 95% of the people affected develop the mildest form: ichthyosis vulgaris.
People usually develop it as children, but some adults experience acquired ichthyosis vulgaris.
The condition usually appears on the legs but can also affect the hands, arms, and trunk.
Symptoms of ichthyosis vulgaris include:
- dry, itchy, and flaky skin
- scaling skin
- mild thickening of the skin
Learn more about ichthyosis vulgaris.
Psoriasis
Psoriasis is a common autoimmune disorder that affects the skin. According to the National Psoriasis Foundation, 125 million people worldwide have the condition.
Doctors are unsure of the exact cause, but it relates to genetics and the immune system.
Psoriasis can affect the entire body, but it is common in the following areas:
- scalp
- face
- palms of the hands
- soles of the feet
- knees
- elbows
- lower back
- genitals
Symptoms of psoriasis include:
- dry, scaly patches of skin that may look violet or purple on darker skin or red on lighter skin
- itchy or painful patches of skin
- peeling skin
- discoloration of fingernails and toenails
A doctor can often diagnose the cause of dry skin patches by examining them, taking a person’s medical history, and asking about risk factors and any skin conditions in the family.
If a physician suspects that the issue results from an underlying medical condition, they will likely refer the individual to a dermatologist, a doctor specializing in skin disorders.
A dermatologist will review the person’s medical history and symptoms and order laboratory tests, such as skin biopsies, to help with a diagnosis.
There are many ways to treat dry skin, including home remedies and medications.
Home remedies
Home remedies for dry skin include:
- exfoliating with a loofah, pumice stone, or scrub to remove dead skin cells, if a doctor recommends it
- applying ointment or cream regularly, ideally using products that contain humectants, ceramides, or emollients
- using a humidifier to add moisture to the air
- applying a cold compress to the affected area
- adding baby oil to warm bath water or applying it when the skin is damp after a shower
- using warm instead of hot water when showering or bathing
- gently patting the skin dry with a towel
- applying moisturizer within 3 minutes of patting skin dry with a towel
Prescription medicines for treating severely dry skin include:
- topical medications, including creams, that contain alpha hydroxy acids or retinoids
- steroids, including hydrocortisone
- antibiotics
- topical antiseptics
- antihistamines
Find more home remedies for dry skin.
Dry skin is usually not a serious health issue, but it can cause discomfort. Chronic or persistent dry skin can indicate an underlying health condition, such as dermatitis, psoriasis, or allergies.
People with dry skin should apply moisturizer regularly and avoid factors that worsen the problem, such as handwashing with harsh soaps.
A doctor can help determine the cause of dry skin patches and recommend treatment. They may make a referral to a dermatologist for more specialist advice.
