We include products we think are useful for our readers. If you buy through links on this page, we may earn a small commission. Here’s our process.
Medical News Today only shows you brands and products that we stand behind.
Our team thoroughly researches and evaluates the recommendations we make on our site. To establish that the product manufacturers addressed safety and efficacy standards, we:- Evaluate ingredients and composition: Do they have the potential to cause harm?
- Fact-check all health claims: Do they align with the current body of scientific evidence?
- Assess the brand: Does it operate with integrity and adhere to industry best practices?
Fibrocystic breast disease refers to breast tissue that feels lumpy and may be painful at times. Fibrocystic breast disease is not a disease, and it is not harmful. Most people now refer to it as fibrocystic breast changes.
Fibrocystic breast changes are common. Some experts estimate they affect between
In this article, learn what fibrocystic breast changes involve, how to get relief, and when to see a doctor.

A person may not need treatment if fibrocystic breast changes cause only mild discomfort. However, options are available to help manage pain.
Drugs and medical treatment
Over-the-counter non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, can provide pain relief. Acetaminophen is another option. Here, learn more about acetaminophen and ibuprofen.
One review analyzed the effectiveness of medications for breast pain. Among the treatments were topical diclofenac gel, a topical NSAID. The results indicated that the gel decreased pain.
If pain is severe and continues longer than
If cysts are large and cause pain, a doctor may drain them.
Heat
Applying a warm compress can help ease pain.
Warm compresses are available for purchase online. People can also make a compress using a towel soaked in warm water or apply a hot water bottle. Be sure not to make it too hot to avoid burning the skin.
How can heat and cold relieve pain? Get some tips here.
Hormonal therapy
Hormone therapy may balance hormone levels and help reduce breast pain.
A doctor may recommend starting, stopping, or
One small study looked at the effect of progesterone gel on symptoms of fibrocystic breast tissue. Using ultrasound, researchers measured the size and number of cysts in 50 people before therapy and during the study. The number and size of cysts decreased during progesterone gel treatment. Those who used it reported a reduction in pain. However,
Wear a supportive bra
A well-fitting, supportive bra will not resolve fibrous tissue, but it may help decrease discomfort. A properly fitted bra should provide support without being too tight. According to one article,
People who are unsure about the best bra size and type may consider seeing a bra-fitting specialist.
Exercise and relaxation
Exercise can boost a person’s overall mental and physical health, and relaxation techniques can reduce stress. Both
Activities that may help include:
Exercise can also help increase lean body mass and reduce body fat, which may help reduce the risk of fibrocystic breast changes, according to a 2018
Examples of relaxation techniques are:
- autogenic training
- progressive muscle relaxation
- deep breathing
Research has not confirmed if dietary factors can affect symptoms of fibrocystic breast changes.
There are no studies that show a casual relationship between caffeine and fibrocystic breast changes. One older review, published in 2004, concluded that high caffeine consumption may worsen symptoms, although the authors noted that the studies involved were small.
There also appears to be no evidence that a low-fat diet will help.
Supplements
Some supplements may help decrease pain associated with fibrocystic breast disease.
A 2018 study divided 94 participants with breast discomfort due to fibrocystic changes into three groups. Each group took one of the following treatments for 6 months:
- two 1,000 milligrams (mg) doses each day of evening primrose oil
- two 50 mg doses each day of vitamin B6
- a placebo
Those who took evening primrose oil or vitamin B6 reported a decrease in pain severity at 1, 2, and 3 months of treatment. There was no reported difference in pain relief between the two supplements, suggesting they may be equally effective.
Research has not confirmed that evening primrose oil is effective, but a doctor
Some
People should check with a doctor before starting a new supplement, as some supplements may not be safe for everyone.
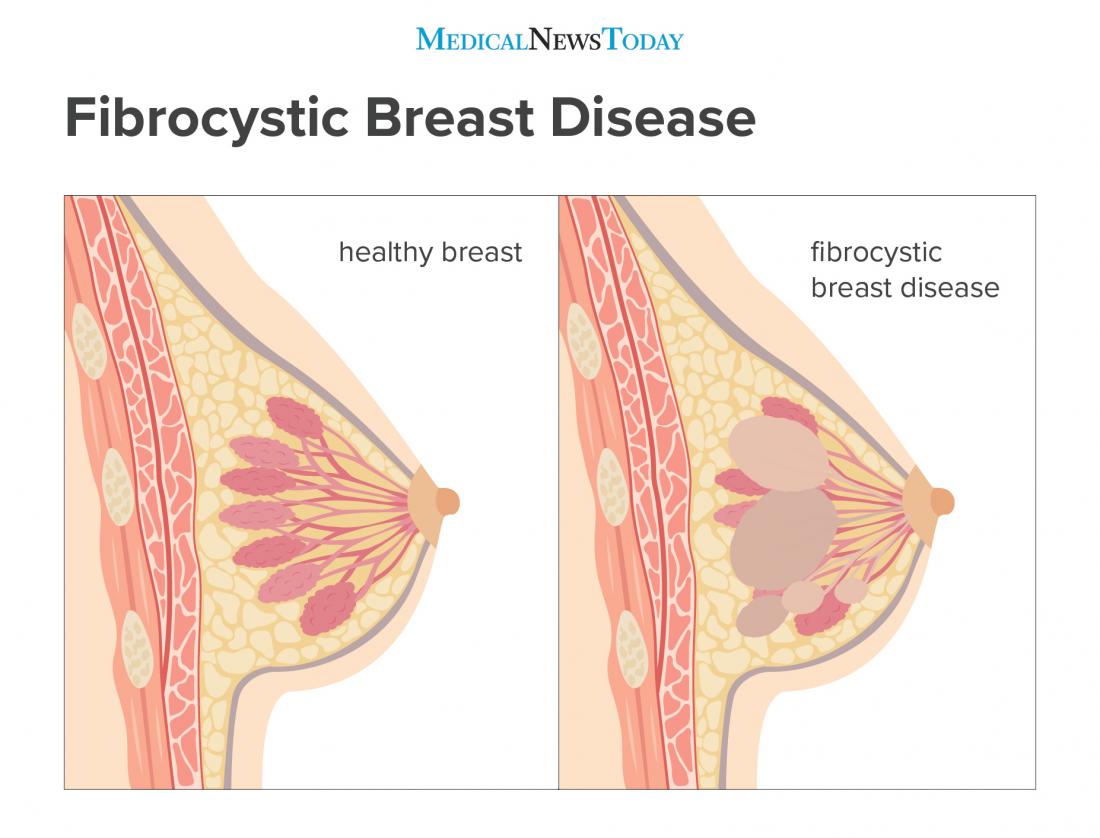
Image credit: Stephen Kelly, 2018
Symptoms of fibrocystic breast disease may come and go during the menstrual cycle. Symptoms may also vary from month to month.
The changes typically occur in both breasts, but lumps and pain may be worse in one breast than the other.
Although it can vary, the pain or discomfort is usually located in the undersides of the breasts or in the upper areas, when the majority of milk glands are.
Typical symptoms
- thickening and lumpiness in the breast
- breast tenderness and pain
- areas of fibrosis that feel rubbery, hard, or smooth to the touch
- a feeling of heaviness in the breast
- swelling
- breast cysts
- nipple discharge
Symptoms may vary during the monthly cycle as hormones fluctuate.
A person should seek medical advice if they notice:
- worsening pain
- new lumps or changes
- dimpling or puckering of the skin
- nipple changes, including a discharge or inverted nipples
- warmth and a change in color
Fibrocystic breast changes are benign, but they
Some breast lumps are cancerous, but many are not. Find out more here.
Fibrocystic breast changes often develop as hormonal levels fluctuate. It is often cyclic, which means it changes with a person’s monthly cycle. Symptoms mostly occur before the age of
According to some experts, using estrogen and progestin treatment after menopause may increase the risk of benign breast changes by
After menopause, a person may experience a sharp or burning pain or soreness in one part of the breast rather than throughout the breasts. This is likely costochondritis, inflammation that affects the rib cage where the bone and cartilage meet. Over-the-counter pain relievers may help.
Experts believe there is a link between hormones and breast changes. Breast tissue responds to fluctuating levels of hormones, especially estrogen. This leads to
People who develop fibrocystic changes may be more sensitive to hormonal fluctuations during the menstrual cycle. It is common for symptoms to become more bothersome right before or during a menstrual period. Taking hormone replacement therapy after menopause may also increase the risk.
A doctor
During the exam, the doctor will feel each breast to check for lumps or abnormal areas. Usually, fibrocystic changes involve lumps that are not attached to the surrounding tissue. The lumps are typically moveable when a doctor palpates them.
Sometimes, a lump may feel firmer than usual, or a doctor may suggest further tests to rule out another condition, such as cancer. Performing a mammogram or breast ultrasound can help them make a diagnosis.
These imaging tests reveal more detail about the breast tissue. If the doctor has concerns, they may recommend a biopsy to rule out cancer.
However, anyone can develop breast cancer, and those with specific types of breast lesions, known as proliferative changes, may have a
For these reasons, everyone should follow a doctor’s recommendations for screening to have a better chance of catching any harmful changes early.
Here, find out more about the early warning signs and when to screen for breast cancer.
Fibrocystic breast changes are a benign condition. They may cause discomfort, but they are unlikely to be cancerous. Doctors do not know the exact cause, but hormones appear to play a key role.
Most people can get relief from over-the-counter or home remedies. If symptoms are severe, a doctor can prescribe treatment. Symptoms usually ease after menopause, but people who use hormone therapy may still experience them.
While fibrocystic breast changes are unlikely to be cancerous, anyone with concerns about changes in their breasts should seek medical advice. Following screening guidance for breast cancer can help identify problems early, when treatment is more effective.
