Lupus is an autoimmune condition that can cause pain, problems in multiple organs and systems of the body, inflammation, and complications that range from minor to life-threatening.
In autoimmune conditions such as lupus, the body’s immune system attacks healthy cells.
According to the Lupus Foundation of America, more than 1.5 million people in the United States have lupus. Around 70 percent have
Systemic lupus erythematosus affects the whole body and can attack virtually any part of it, including skin, major organs, hair, muscles, joints, and the digestive system.
Most people with lupus receive a diagnosis between the ages of 15 and 44. Only around 15 percent of people experience symptoms of lupus before the age of 18.
Demographic and other factors can affect the severity and progression of the condition. Lupus is most prevalent among women of childbearing age, and it is “two to three times more prevalent among women of color,” according to the Lupus Foundation of America.
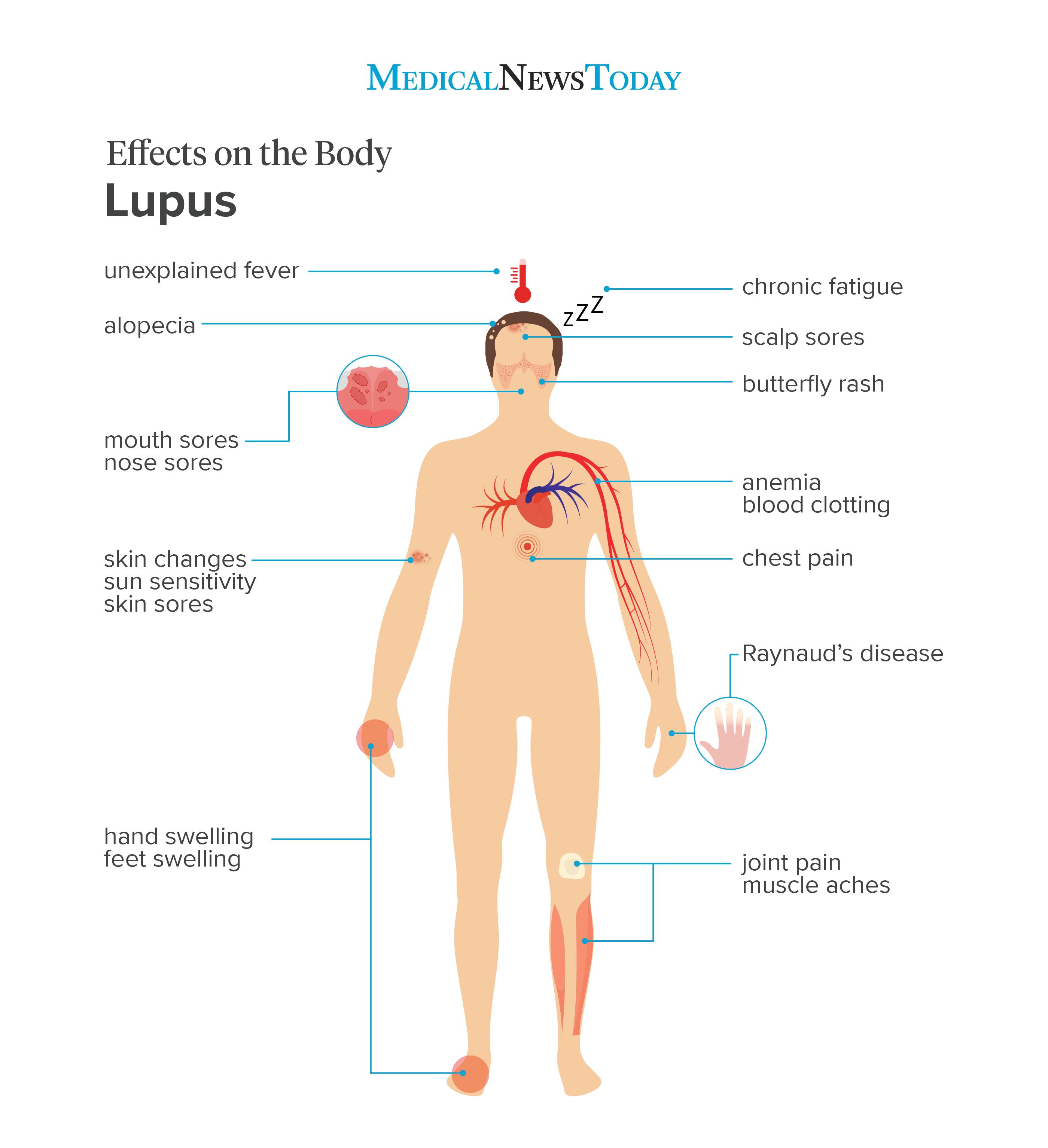
Lupus may cause symptoms that are subtle at first but get progressively worse. The symptoms may also appear suddenly or gradually.
Many people with lupus do not receive a diagnosis straight away because it can mimic other conditions, including fibromyalgia, rheumatoid arthritis, and various others that affect the same organ systems.
Virtually any symptom of illness or inflammation can signal lupus. However, some of the symptoms most closely associated with lupus include:
- a butterfly-shaped rash on the face
- skin changes and sun sensitivity
- an unexplained fever
- joint pain and chronic muscle aches or pain
- hair loss or alopecia
- fingers that turn lighter when cold (Raynaud’s disease)
- anemia
- swelling in the hands and feet
- chest pain when taking a deep breath
- chronic fatigue
- sores in the mouth or nose
- sores on the scalp
- abnormal blood clotting
There are other types of lupus beside systemic lupus erythematosus. Other types include:
Cutaneous lupus
Some people develop cutaneous lupus, which affects areas of sun-exposed skin. There are
Symptoms include:
- a butterfly-shaped rash on face
- scaly, circular raised patches that resemble psoriasis lesions
- a red-purple rash on the head, face, and ears
Exposure to sunlight can make these types of lupus worse. Some people with skin lupus may develop lupus inside their body, too.
Neonatal lupus
Some babies are born with neonatal lupus, which occurs when the mother’s antibodies attack the baby. Typically, the mother and baby do not have systemic lupus erythematosus, though some women may develop it later on.
Symptoms include:
- a butterfly-shaped rash on face
- liver problems
- anemia
Neonatal lupus usually disappears within 6 months.
Over time, lupus can lead to severe complications. Such complications may include:
- organ failure
- infections and other autoimmune issues
- chronic pain and fatigue
- breathing difficulties due to inflammation in the lungs
- congenital heart block in babies
- an enlarged head (macrocephaly) in babies, though this is rare
No single test can diagnose lupus. Instead, a doctor must look for signs of systemic inflammation, which indicates that the immune system may be attacking the body.
To help with diagnosis, doctors may:
- take a complete medical history, including a log of all symptoms and how they have changed over time
- take a family medical history
- conduct blood tests to rule out other conditions and to look for signs of systemic inflammation
- carry out an antinuclear antibody test, which is a blood test that looks for signs of autoimmune conditions but which cannot specifically diagnose lupus
In some cases, a doctor may recommend waiting to see how and whether symptoms change over time.
Lupus is a chronic condition. There is currently no cure, but there are some treatments that can help a person manage their symptoms and prevent serious complications.
The right treatment varies from person to person, and a person’s treatment needs may change with time. Sometimes, a medication that once worked well stops working or begins to cause severe side effects.
For these reasons, it is essential to work with a healthcare professional to develop a comprehensive treatment plan.
The
- Immunosuppressant drugs: These drugs suppress activity in the immune system and reduce its ability to attack the body. They can be effective but may increase a person’s risk of developing serious infections.
- Pain relief medications: Prescription and over-the-counter (OTC) pain medications, especially nonsteroidal anti-inflammatory drugs such as ibuprofen, may help with chronic pain.
- Corticosteroids: Steroids can reduce swelling and pain. OTC steroid creams may help with skin symptoms. A doctor can also prescribe steroid pills or shots to help with systemic symptoms.
- Anti-malaria drugs: Hydroxychloroquine and chloroquine phosphate may help with lung inflammation, joint pain, and rashes.
- BLyS-specific inhibitors: These drugs prevent people from developing abnormal B cells, which are immune system cells that create antibodies.
- Medications for symptoms: A healthcare professional may prescribe other medications based on a person’s symptoms. For example, a person might need to take osteoporosis or high blood pressure drugs. Taking blood thinners can also reduce the risk of a blood clot.
Scientists are researching other strategies for treating lupus. Clinical trials offer hope to some people with the condition, so it may be worth asking a doctor whether any trials are taking place locally.
Some people with lupus find relief from alternative remedies, such as acupuncture and special diets. Clinical research has not yet found solid evidence to suggest that these treatments work. However, trying them in conjunction with other treatments is harmless.
Many people with lupus find it challenging to live with. Some people might struggle with anxiety about their long-term outlook or feel as though they have little control over their body or life.
Chronic pain and fatigue can be debilitating, making it difficult to work. This can cause financial woes that make some treatments inaccessible.
Support groups can help people with lupus talk through their emotions, feel less isolated, and uncover potentially effective treatment options.
Some people also find relief from psychotherapy and other strategies to improve mental health.
Below are frequently asked questions relating to the early signs of lupus.
Can lupus be detected by blood test?
Doctors use many different tests and symptom assessments to diagnose lupus. Blood tests form part of this overall assessment but alone cannot typically diagnose lupus.
What are the 11 criteria for lupus?
The 11 criteria of lupus are:
- malar rash
- discoid rash
- photosensitivity
- oral ulcers
- serositis
- arthritis
- renal disorders
- neurological disorders
- hematological disorder
- immunologic disorder
- presence of anti-nuclear antibodies
However, the European League Against Rheumatism (EULAR) and the American College of Rheumatology (ACR) published new criteria for the classification of lupus that differ from these 11 points.
What are the warning signs of lupus?
People may experience lupus symptoms at different times and in different severities. However,
- rashes
- fever
- muscle and joint pain
- chest pain
- mouth sores
Is it MS or lupus?
Multiple sclerosis (MS) can cause symptoms similar to lupus. However, MS affects the central nervous system, while lupus directly affects the skin, joints, and other tissues. Both conditions can cause:
- fatigue
- localized pains
- weakness
Typically MS does not cause rashes, whereas these are common lupus symptoms. By contrast, vision problems, numbness, tingling, and coordination issues are hallmarks of MS, but not lupus.
Learn more about the similarities between lupus and MS here.
Despite the fact that there is currently no cure for lupus, there are many potentially effective treatments. People with lupus can live long and happy lives. Also, women with the condition can have successful pregnancies.
People who suspect that they may have lupus should seek prompt treatment. The longer it progresses untreated, the more likely it is to cause serious complications.
A doctor who is knowledgeable about lupus is the best ally in its treatment, so choose a doctor who listens and cares.
