Patients with atrial fibrillation who have a coronary stent placement and are on anticoagulation therapy may drop the aspirin and just take clopidogrel (Plavix) plus their anticoagulant medication, researchers from the TweeSteden Hospital, Tilburg, the Netherlands, explained at the European Society of Cardiology Congress in Munich, Germany. Patients with heart rhythm disturbances, such as those with atrial fibrillation and/or mechanical valves, usually need anticoagulation therapy for life in order to prevent stroke.
The researchers of the WOEST study said that dropping aspirin from the antiplatelet regimen does not compromise their safety; their risk of bleeding is still reduced.
People who have had a coronary stent placement usually take clopidogrel alongside aspirin to protect against the risk of stent thrombosis, a rare but life-threatening complication.
Patients with coronary heart disease may have had a buildup of cholesterol and fatty deposits (plaques) in the inner walls of the arteries, which restrict blood flow to the heart muscles. A coronary stent can resolve the plaque blockage and restore bloodflow to the heart muscles. A procedure called PCI (percutaneous coronary intervention) is used.
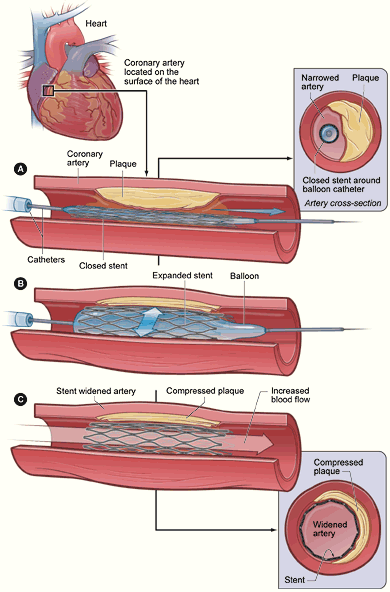
Stent placement. A. A catheter is inserted into the lesion. B. The balloon is inflated, compressing the plaque and expanding the stent. C. After removing the catheter and deflated balloon, the expanded stent remains and blood flows through the holes in the mesh.
Patients with atrial fibrillation or a mechanical valve who take anticoagulant medications and also undergo coronary stenting usually take clopidogrel, aspirin and oral anticoagulants to prevent stent thrombosis and stroke. However, Dr Willem Dewilde said nobody knows what their optimal antithrombotic treatment is.
The problem with taking all the three drugs at the same time is that the risk of serious bleeding is considerably increased. Many patients end up having to stop taking the clopidogrel and aspirin.
Dr Dewilde explained that the results from the WOEST study (What is the Optimal antiplatElet and anticoagulant therapy in patients with oral anticoagulation and coronary StenTing) have demonstrated that dropping the aspirin, and keeping the clopidogrel and anticoagulants results in less bleeding, but is also safe and still prevents such complications as stent thrombosis.
Dr Dewilde said:
“WOEST is the first study demonstrating that the omission of aspirin in patients treated with oral anticoagulants and having a coronary stent is safe”.
The study’s aim was to resolve this dilemma – what is the ideal antithrombotic treatment those on oral anticoagulant medications who have to undergo coronary stenting? Before WOEST began, the researchers had hypothesized that the omission of aspirin would be the solution. It appears they were right.
Dr Dewilde said:
“This would possibly lead to less bleedings, but hopefully would not increase the risk of thrombotic complications such as stent thrombosis.”
WOEST consisted of 573 patients who were already on oral anticoagulants for atrial fibrillation or mechanical valves. They were all undergoing coronary stenting. The participants were randomly selected into two groups:
- Double therapy group – they were given additional clopidogrel only (no aspirin)
- Triple therapy group – they were given additional clopidogrel and aspirin
The study, which lasted from November 2008 to November 2011, was conducted in 15 hospitals in Belgium and the Netherlands.
They found that those in the double therapy group had less bleeding and a lower overall mortality rate after 12 months compared to the participants in the triple therapy group. They also reported no higher incidences of stent thrombosis or myocardial infarction in the double therapy group.
Dr Dewilde said:
“Thus, the WOEST study demonstrates that omitting aspirin leads to less bleedings but does not increase the risk of stent thrombosis, stroke or myocardial infarction. Although the number of patients in the trial is limited, this is an important finding with implications for future treatment and guidelines in this group of patients known to be at high risk of bleeding and thrombotic complications.”
Atrial fibrillation is when the speed or rhythm of the heart beat is wrong, usually too fast. It is caused by a fault in the heart’s electrical system. Atrial fibrillation is the most common type of arrhythmia (irregular heart beat).
The two upper chambers of the heart are called the atria (left atrium and the right atrium). The two lower chambers are called the ventricles (left ventricle and right ventricle). A patient has atrial fibrillation when the atria contract too fast and irregularly.
The signs and symptoms of atrial fibrillation may include dizziness, lightheadedness, confusion, palpitations, breathlessness, chest pains (during exertion), angina, hypotension (low blood pressure), weakness, confusion, disorders of the heart muscle, and heart failure. Some patients have no symptoms and only find out they have the condition during a routine examination.
Written by Christian Nordqvist