We all know that smoking is bad for our health. But how bad is bad? The answer is very bad, life changing in fact. But everyone also knows someone who has smoked all their adult life, never gotten lung cancer or a respiratory disease of any kind and lived to a ripe old age. George Burns, the famous comedian, who lived to be 100 hundred years old, often remarked “I smoke ten to fifteen cigars a day. At my age I have to hold on to something”.
So, true enough – but in the discussion ahead you will find that these individuals are very much the rare exception and certainly not the rule. It is important to know that, on average, smokers die twelve years sooner than non-smokers. Twelve years! That’s more than a decade! It means life for smokers is more than ten percent shorter than for non-smokers. These are big numbers.
Is this just fear mongering or is there substance to such a statement? It is real. The data is in and it is very strong.
No other preventable cause of illness or death is more important than smoking. This is the clear message of two new studies that investigated the overall impact of smoking across a very large cohort of Americans. The studies, conducted by Jha et al1 and by Thun et al 2 along with an editorial by Schroeder3, were published by the New England Journal of Medicine on January 24, 2013. They support earlier studies that came to similar conclusions based on smaller numbers of observed individuals.
So, here are the facts of the matter. According to the National Cancer Institute (NCI), tobacco is the leading cause of preventable illness and death in the United States and that, in 2011, an estimated 19 percent of U.S. adults were cigarette smokers.4 This is down from over 40% a few decades ago. Good progress. But for those who do smoke, diseases leading to death are common.
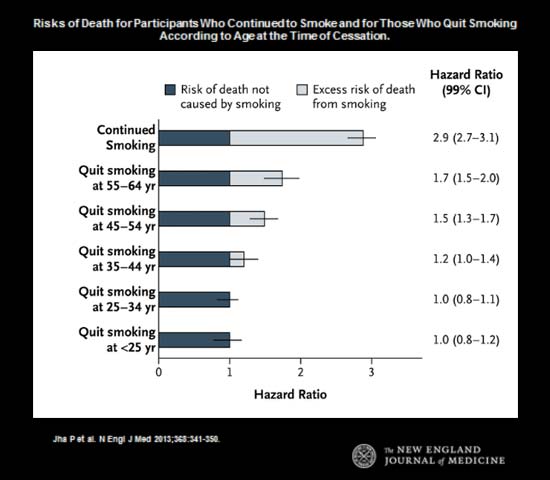
Smoker’s mortality rates are nearly 3 times greater than those of nonsmokers and essentially equal between men and women. People who smoke are up to six times more likely to suffer a heart attack than nonsmokers, and the risk increases with the number of cigarettes smoked. Cigarette smoking causes an estimated 443,000 deaths each year, including approximately 49,000 deaths due to exposure to secondhand smoke.
Smoking also causes most cases of chronic obstructive lung disease. Lung cancer is the leading cause of cancer death among both men and women in the United States, and 90 percent of lung cancer deaths among men and approximately 80 percent of lung cancer deaths among women are due to smoking currently or in the past. Certain diseases, such as ischemic heart disease (heart attacks and related coronary artery disease), stroke, chronic lung disease and lung cancer, have been clearly linked to smoking and were found to be the cause of death in approximately 60% of the smokers’ in these studies.
Smoking causes or predisposes to many other types of cancer, including cancers of the throat, mouth, nasal cavity, esophagus, stomach, pancreas, kidney, bladder, and cervix, and acute myeloid leukemia.
The chance that a young person will live to age 80 is about 70% for nonsmokers but only 35% for smokers. Stated differently, a smoker loses about 11(women) to 12 (men) years of life compared to nonsmokers. Sadly, the NCI’s 2011 report confirms that nearly 16 percent of high school students smoke cigarettes.
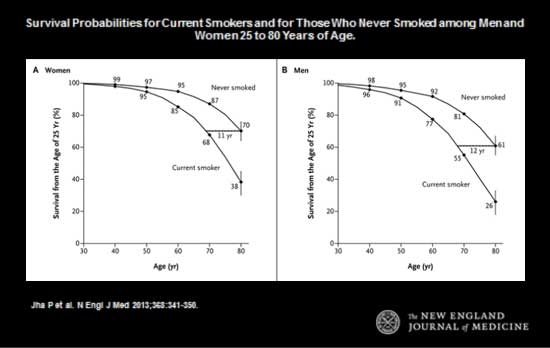
 The Thun Study
The Thun study compared data from three time periods reaching back 50 years. Overall, mortality rates during this fifty year period declined by 50%; largely as a result of the progress against heart disease. However, this was a benefit enjoyed solely by the nonsmokers.
Thun made some key observations:
- Smoking deaths continue to increase among women because women who smoke now smoke as much as men do
- Death from all causes is at least 3X higher for smokers than for nonsmokers with at least two thirds of all deaths in smokers directly related to smoking
- The rate of death from chronic lung disease (COPD) is rising among both men and women. They hypothesize that this rise in incidence is related to the changes in cigarettes over the years that encourage deeper inhalation; consequently delivering more toxins to the deep, peripheral regions of the lungs – the alveoli or air sacs.
Using the same reasoning, they suggest that deeper inhalation than in the past may be causing the increased incidence of peripheral lung cancers, especially adenocarcinomas, versus the more centrally located and mostly squamous cell cancers that were more common in the past.
- Quitting smoking lowers death rates quite substantially and quitting before the age of 40 can eliminate the relative risk of early death.

The Jha Study
In the Jha study, the increased risk for ischemic heart disease among smokers compared to nonsmokers was about 3.5 times (i.e., smokers had 3.5 times as many deaths from heart disease as did the nonsmokers). Since heart disease is more frequent than lung cancer or chronic lung disease, this represented a large and common cause of death for smokers.
Considering just females for example, among the 23,839 women who smoked in the study, 251 died of heart disease compared to 382 of the 67,574 women who never smoked. Lung cancer caused fewer total deaths, but the relative risk for smokers was very high – 18 – based upon 289 women who smoked and died of lung cancer compared to 83 lung cancer deaths for the larger number of women who never smoked.
These two studies are a stark reminder that smoking is not simply a health hazard. Smoking directly leads to an extraordinary increase in the risks of death from heart disease, stroke, chronic lung disease and lung cancer, among others. In the Jha study, 62% of the smokers’ deaths were attributable to smoking.
Smoking in the military provides a further microcosm of evidence that supports the studies of Jha et al and Thun et al. Studies investigating cancer incidence in the military have indicated higher rates of lung cancer incidence and mortality among veterans than non-veterans.5 6 7 8
The most comprehensive analysis of the prevalence of cancer in the 9.3 million military beneficiaries covered by the Military Health System and Tricare showed that the rate of lung cancer may be twice as high in the military population than the lung cancer prevalence rate for the entire population.
Until 1976, cigarettes were routinely issued to military personnel as part of their meal supplementation, known as K-rations and C-rations, and were for decades sold at deeply discounted prices in commissaries and exchanges to military personnel, their families, defense contractors and civilian workers. They were part of the service men and women’s rations during World War II and the Korean War.
Tobacco products are still sold at discounted prices on military exchanges and commissaries, with the exception of Navy and Marine commissaries.

According to a retrospective study that analyzed the cause of death data for people born between 1920 and 1939, the mortality rates for lung cancer among veterans has been nearly twice that of civilians. 2,000,000 World War II and Korean War veterans died an average of 11.1 years sooner than their civilian counterparts, making the toll of premature deaths in terms of “years of life lost” greater than that of all combat casualties from both wars. This points to yet another confirmatory data point in support of Jha et al and Thun et al’s finding that smoker’s life spans are cut short by over a decade.
The percentage of active duty military who ever smoked was highest during the Korean and Vietnam Wars (75%). Currently, 32% of active duty military personnel smoke versus 20% of adults in the civilian population and 22% of veterans.
Studies carried out by the Australian Veterans Administration found a 47% higher rate of lung cancer among its veterans who participated in the Korean War and double the rate of lung cancer cases among Australian veterans who served in Vietnam. These veterans had lung cancer mortality rates 79% higher than expected in the general Australian population.
Clearly, military personnel are subject to increased risk factors from a wide variety of causes and exposures. For example, many have been exposed to radon, asbestos, beryllium, fuel exhaust and other battlefield emissions. Some Vietnam veterans were exposed to Agent Orange, a herbicide used to kill vegetation in the jungle. Gulf War veterans were exposed to depleted uranium used in weapons and armor shielding. Depleted uranium ordinance is being found to cause obstructive bronchiolitis within months or years of exposure. So, it is acknowledged that the increased incidence of pulmonary disease and lung cancer among the veteran population certainly has compounded exposure factors beyond just smoking.
However, studies on the incidence of pulmonary disease and lung cancer in the military population suggest that these other exposures are/were intermittent at best and that smoking as part as of the military personnel’s day-to-day lifestyle accounts for a significantly higher percentage of the lung cancer rates seen in the military population than those being reported in the civilian population, accounting for as many as 50-70% of the deaths. The popular phrase “Smoke if you got ’em” was coined from the battlefield.
With this background, what are the specific hazards of tobacco? The big three are lung cancer, heart disease and chronic lung disease (i.e. emphysema and chronic bronchitis which together are known as chronic obstructive pulmonary disease or COPD). In terms of individual risk, smoking increases the risk of coronary heart disease by about 2-4 times, lung cancer by 23 times, and COPD by 12-13 times. As stated earlier, it is important to realize that since coronary artery disease is comparatively common, doubling or quadrupling the risk is a very large number of additional people who get coronary artery disease who smoke. Although lung cancer is not nearly as common, when the risk goes up 23 times it does become common. The same goes for COPD. And once these diseases develop, they remain for life. Coronary artery disease and COPD can be treated, but not cured. The clock cannot be turned back. As for lung cancer, a few are cured today. And despite major advances in diagnosis and treatment, most individuals who develop lung cancer die within a few years. (For a broader discussion of lung cancer, see The Future Of Healthcare Delivery For Lung Cancer published in Medical New Today on Feb 15, 2013 and available at http://www.medicalnewstoday.com/info/lung-cancer/future-of-healthcare-overview.php ). 85% of all those who get lung cancer perish within just five years of their diagnosis. Unlike many other cancers, lung cancer mortality has not changed since the mortality rates for all cancers were first published by the NCI in 1976.
There are other diseases caused or exacerbated by tobacco smoking including stroke and narrowed arteries to the legs and feet. It also is a major causative factor for abdominal aortic aneurysms (which is a “ballooning” of the aorta which can rupture and lead to rapid death.)
Some of the other cancers caused, at least in part, by tobacco smoking are some leukemias and cancers of the throat, mouth, nasal cavity, esophagus, stomach, pancreas, kidney, bladder, and cervix.
Smoking has been linked as a causative factor in the rapid loss of calcium to the bones of post-menopausal women, effectively leading to greater osteoporosis and hence more hip fractures in older individuals.
Smoking during reproductive years can mean infertility and premature births.
Overall, smoking accounts for about 1 in 5 (20%) of all deaths in Americans or 443,000 deaths in the United States per year.
These are all preventable outcomes, meaning that smoking is the most preventable cause of death and disease in the United States today. It is rapidly becoming more significant in less developed countries. Today, there are about 40 million Americans who smoke, but internationally the total is about 1.3 billion. Mostly these smokers live in the developing world where the percentage of smokers is high and rising. There is, unfortunately, no suggestion that the initiation of smoking is declining, indeed it is still increasing. Jha et al estimated that “on the basis of current rates of smoking initiation and cessation, smoking, which killed about 100 million people in the 20th century, will kill about 1 billion in the 21st century.”
Smoking harms women and men equally – It had been thought that women were somehow less affected than men by tobacco smoke. That is simply not true. There is no gender gap. “Women who smoke like men die like men who smoke.” Both men and women who smoke have an increased risk of acquiring lung cancer 25 times that of non-smokers.
The history of smoking in America explains why the “gender gap” was a mirage. Once the machine manufacturing of cigarettes began in the early 20th century, men picked up the habit, especially in the aftermath of World War I. For women, smoking was largely considered socially unacceptable at that time. Since it takes 20 to 30 or more years to induce the various smoking-related diseases, men began to develop lung cancer, symptomatic COPD, recognized coronary artery disease and so on only after World War II. And as more and more men smoked more and more cigarettes per day, for more than 20-30 years, the rates of these diseases began to increase rapidly in the 1960’s and 1970’s.
Women only began to smoke regularly after World War II and as manufacturers began to specifically target their advertising to women, with brands like Virginia Slims. So, in the 1960’s and 70’s the increased rates of these diseases had not yet appeared in women. Hence the “gender gap” seemed to be in effect. However now, the rates of disease are the same for anyone who has smoked many cigarettes per day (or packs per day) for many years.
How does smoking harm health?
Tobacco has more than just nicotine and tar in its smoke. Over 4,000 chemicals have been detected in smoke and perhaps 250 are proven harmful according to the Centers for Disease Control (CDC). Among them are some commonly known chemicals like arsenic, benzene, cadmium, chromium and formaldehyde.
Carbon monoxide is also released in tobacco smoke and binds up the hemoglobin in the red blood cells that normally carry oxygen. Carbon monoxide also affects arteries and speeds up the process of coronary artery disease or atherosclerosis.
Nicotine is highly addictive and also has a narrowing effect on arteries including coronary arteries.
Secondhand smoke – If it takes heavy smoking for many years to lead to high rates of disease then can secondhand smoke be much of a problem? The answer is definitively and definitely yes.
Secondhand smoke is especially dangerous to children who will develop more respiratory infections and many will later progress to the same diseases as direct smokers, albeit in lower numbers.
It is estimated that the risk of coronary artery disease goes up by about 25-30% among those exposed to secondhand smoke compared to those who are not exposed. The result is that, as the NCI reported, nearly 50,000 people die from coronary artery disease each year as a result of secondhand smoke along with about 3,500 dying of lung cancer.
The first public pronouncement that tobacco smoking was harmful to society’s health was by Luther L. Terry, M.D., Surgeon General of the U.S. Public Health Service in 1964. This report was aggressively criticized, especially by the tobacco companies and their proxies. Still, it rapidly led to Congress mandating warnings on cigarette packages of the harmful effects of smoking on health and the banning of radio and TV advertising.
More than twenty years later, Dr. C. Everett Koop, the Surgeon General from 1981 to 1989 took a strong stance on the health hazards of tobacco. A pediatric surgeon, he had been an active opponent of abortion, speaking against it around the country before his nomination and hence had strong support in the Senate from many conservative senators from the South, including tobacco growing states. But Koop soon made tobacco his top public health enemy. Smoking he said was “the most important public health issue of our time.” He made it a truly national issue, used his bully pulpit to get on radio and TV and emphasize the dangers of secondhand smoke. His early Senate supporters in tobacco states quickly lost their affection for him, but he felt it was a moral responsibility to speak out forcefully.
Today about 19% of Americans smoke, down from over 40% a few decades ago. That is to the good. The bad news is that among those who smoke a large proportion are younger – ages 18-35. In the past, smoking was prevalent among the more educated, white collar employee. Today it is more prevalent among the less educated, more socioeconomically stressed individual. Not only are rates high and even rising in this group, but so is the amount smoked.
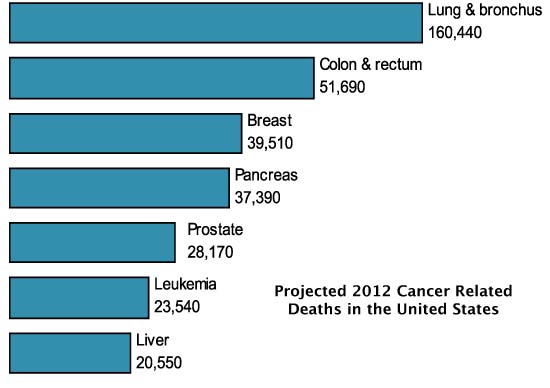
Source: American Cancer Society, Inc. Surveillance Research – 2012
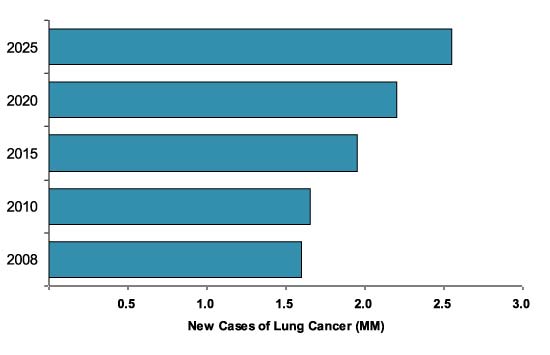
Source: World Health Organization, Global status report on non-communicable diseases – 2010
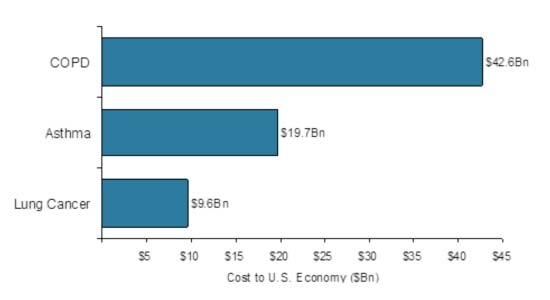
The Centers for Disease Control (CDC) looked at consumption over the past decade. From 2000-2011, the total “combustible tobacco” consumption declined from 450.7 billion cigarette equivalents to 326.6 cigarette equivalents or a 28% decline. Put that as a per capita figure and it declined from 2,148 to 1,374 cigarette equivalents or a 33% decline. Machine made cigarette consumption declines accounted for most of this change. However, other combustible tobacco products (i.e. cigars, pipe, and roll-your-own tobacco) actually increased 123%, a real concern. These components represented only about 4% of the total in 2000, but now amount to about 10%.
Of course, it does not matter what a person smokes – cigarettes, pipe, or cigar – they all release the same toxins into the lungs. Why this small but increasing switch to these other products? Mostly it has to do with tax law. Cigarettes are highly taxed making them expensive; pipe tobacco and “large” cigars are lightly taxed, making them relatively less expensive. Manufacturers have therefore relabelled loose roll-your-own tobacco (highly taxed like cigarettes) as pipe tobacco so as to benefit from lower taxes. Similarly, “small” cigars are highly taxed like cigarettes, but just a slight increase in size makes them into lightly taxed “large” cigars even though they otherwise resemble typical cigarettes in size.
Not surprisingly, a new Surgeon’s General report in 2012 notes that youth and young adults have a higher use rate of cigars and other more lightly taxed combustible tobacco products.
The economic realities of smoking do not stop there, either. The cost of smoking-related disease is a significant cost burden on the Gross Domestic Product of the US economy. Of the $2.2 trillion the US spends on health care, annually, $1.1 trillion of that spend is related directly to the cost burdens of chronic non communicable diseases. Of this $1.1 trillion cost burden pulmonary disease and lung cancer account for $154 billion. Nearly 15%! The cost of heart disease and stroke accounts for a $444 billion cost burden.
A quick extrapolation of the statistics from Thun et al and Jha et al would relate that smoking related diseases, associated with just lung, heart and vascular ailments, pose an economic cost burden to the US GDP in the hundreds of billions of dollars, annually. So, both the humanitarian and financial consequences of smoking and tobacco certainly cannot be overstated.
It is well understood that tobacco is addictive and that smoking is easy to start and hard to quit. Many try each year only to go back on. If someone has smoked for a long time, does it make any difference or is it just too late? What value does quitting smoking have, if any in these circumstances? The answer is that quitting is exceptionally valuable and it is never too late to have a meaningful effect.
Those who quit smoking will gain back substantial years of life, with more years gained the sooner one ceases smoking. For example, in Jha’s analysis, those who quit in the age range 25-34 reverted almost to the nonsmoker status – they gained back 10 years of life. Stopping between 35-44 years of age gained 9 years and between 45-54 years of age the gain was 6 years. So it is always a good time to quit.
 Quitting today is the single most important step a smoker can take to improve their health over the years to come. Some argue that if they quit they will gain weight and that will make them more susceptible to diabetes mellitus or coronary artery disease. A possibly logical argument, but the data is in – quitting may lead to some weight gain, but it is hardly enough to have a significant or serious impact and so does not – by far – overcome the benefits of smoking cessation. Moreover, it is an argument that fails in comparison to the extension of one’s life.
Quitting is difficult. No question. Nevertheless, it is well worth it! The best approach is to use a combination of techniques all at once. Counseling by the patient’s physician and augmented by a professional cessation counselor can have a major impact. Nicotine patches can help slowly and gently ease one off of the nicotine addiction. Support groups, whether they be real or virtual, in person or via social media can be very helpful; after all, each person in the group is going through the same difficult transition. Incentives help as well as a strong family and friends’ support system. Workplace tobacco cessation programs are very useful and if one is not available many health departments can make a referral. The success of quitting goes way up when these and other techniques are used together, rather than just trying to quit “cold turkey” on one’s own.
To assist an individual, the provider (physician, nurse, nurse practitioner) needs to follow the Public Health Service “5As” model:
- Ask each patient if they smoke
- Advise all smokers to quit
- Assess the smoker’s willingness to quit (readiness)
- Assist with the quitting
- Arrange appropriate follow-up contact both with the provider and others such as counselors
This all takes some time, but it is essential to high rates of success.
A concept called self-efficacy is important here. Those with low self-efficacy are those with low personal expectations that they will be successful at quitting. Their relapse rate is higher so they need to be identified early and offered special assistance.
Often not recognized by the general population is the value of smoking cessation before a surgical procedure. Smokers have higher rates of complications during and after surgery than do nonsmokers. For elective procedures many surgeons now insist on cessation for some month’s pre surgery. This is a good idea which needs to be augmented post-surgery to prevent later relapse.
Fortunately, there have been active efforts for many years to warn of the dangers of smoking and to assist individuals to quit. However, smoking has become a stigmatized behavior so that those who smoke are shunned and those who develop smoking related illnesses like lung cancer are stigmatized (“you brought it on yourself”) as well.
Lung cancer kills more women than breast cancer, but there is no “Pink Ribbon” Campaign or “Race for the Cure.” Women have proven themselves to be the best advocates for a healthy society. Women’s leadership in the fight against breast cancer has been the single best disease advocacy and funding initiative ever seen. The reality is that lung cancer killed 74,000 women in 2010 as compared to the 38,000 lost to breast cancer. Nearly twice as many women were lost to lung cancer in 2010 than breast cancer.
So, where are the voices? There is a compelling case to be made for a renewed focus on prevention and treatment of pulmonary disease and lung cancer, in particular. Over 96 million Americans have admitted to smoking for at least six months during their lifetime, an exposure rate that puts one third of America’s population at least at some level of risk.
So, why be prejudiced toward those with pulmonary disease and lung cancer? The fact is that we are all paying for the cost burden of smoking on our society in real dollars and in real lives. There is a significant need for a nonjudgmental attitude toward those who are afflicted. Getting past the “blame game” removes the stigma and allows a more constructive approach to tobacco cessation and disease prevention and treatment.
Attempts to curtail the initiation of smoking, to assist with smoking cessation and to increase the focus and expedite the research initiatives to treat and cure smoking related diseases are perhaps the most important health promotion and disease prevention goals for America at this time.
If there is any single message to take away from the new information on tobacco usage it is this – Tobacco is the single most important cause of preventable disease and death. It is never too late to quit and the benefits of quitting are clearly substantial. Gaining back a decade of healthy life is a very real and achievable goal.
About the Authors
Stephen C. Schimpff, MD, a professor of medicine and public policy, retired CEO of the University of Maryland Medical Center, chair of the Sanovas, Inc. scientific advisory committee, senior advisor to Sage Growth Partners and is the author of “The Future of Health Care Delivery: Why It Must Change And How It Will Affect You.” Larry Gerrans is an inventor and developer of medical technologies. He is the Founder and CEO of Sanovas Inc., a Life Science Technology Company dedicated to the early detection and treatment of serious chronic illnesses including lung cancer, asthma and chronic obstructive pulmonary disease (COPD).
Written by Stephen C Schimpff, MD and Larry Gerrans
