Premenstrual syndrome (PMS) refers to the physical and psychological symptoms that a person may experience before their menstrual period. These can include bloating, headaches, mood changes, and more.
Headaches, bloating, cramps, and mood swings are among the most common PMS symptoms. For some, these symptoms are a minor inconvenience. For others, the symptoms can be so severe that they miss work or school.
Most females experience some degree of PMS. In fact,
In this article we look at PMS, including its symptoms, causes, treatments, and tips for coping. We also discuss when a person should see a doctor about their symptoms.
PMS refers to the diverse range of physical and psychological symptoms that people experience before their menstrual period.
The exact cause of PMS remains unknown. However, natural fluctuations in hormone levels, especially those of estrogen and progesterone, in the week or two before menstruation are likely responsible for the symptoms.
Estrogen and progesterone levels decrease dramatically after ovulation. This could play a major role in the development of PMS symptoms.
The drop in estrogen levels may affect a person’s serotonin levels. Serotonin is a brain chemical that helps regulate mood, sleep, and appetite, all of which PMS affects.
Severe or debilitating PMS symptoms are not common, and they may indicate the presence of an underlying health condition. Speak to a doctor about any severe PMS symptoms.
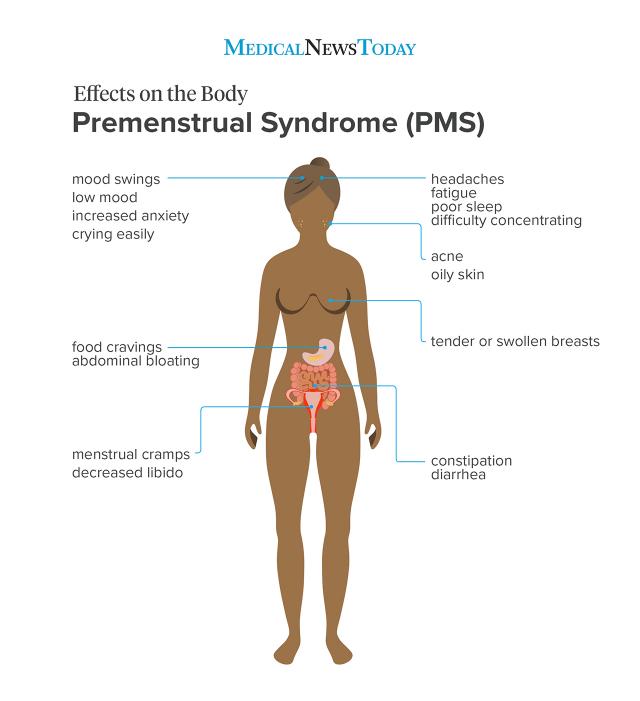
Image credit: Stephen Kelly, 2019.
PMS symptoms range from mild to severe. Some people get their periods without experiencing any PMS symptoms at all.
For other people, however, PMS symptoms can significantly affect their ability to perform regular activities and may even reduce their quality of life.
Physical symptoms of PMS can include:
- changes in appetite, such as food cravings
- tender or swollen breasts
- weight gain
- abdominal bloating
- pain in the lower abdomen or menstrual cramps
- constipation or diarrhea
- headaches
- fatigue
- oily skin
- acne, pimple breakouts, and other skin symptoms
Psychological symptoms of PMS can include:
- low mood
- feeling tearful or crying
- irritability or anger
- depression
- increased anxiety
- mood swings
- social withdrawal
- problems sleeping, such as insomnia
- difficulty concentrating
- decreased libido
In PMS, people may also notice that the symptoms of conditions such as diabetes, depression, and inflammatory bowel syndrome worsen.
Also, age can affect the severity of PMS. During perimenopause, which is the transitional period leading up to menopause, people
People may not realize straight away that their symptoms are related to menstruation, especially if they have an irregular cycle.
Keeping a diary of when symptoms occur can help a person notice patterns. If symptoms occur at roughly the same time each month, or at the same stage in a person’s menstrual cycle, they may be due to PMS. If not, the symptoms may have another cause.
Severe or debilitating PMS symptoms are not common. Speak to a doctor if PMS symptoms get in the way of daily life. In some cases, severe symptoms may indicate premenstrual dysphoric disorder (PMDD) or another medical condition.
Some conditions affecting the reproductive system, such as endometriosis and polycystic ovary syndrome, can cause severe PMS. A doctor can help treat these conditions and reduce a person’s symptom frequency and severity.
People may want to consider seeing a doctor if their PMS symptoms do not improve after trying over-the-counter (OTC) medications, home remedies, or lifestyle changes.
Sometimes, taking hormonal contraception can give rise to PMS-like symptoms. This is because these drugs change the levels of hormones in the body.
These symptoms may be less predictable depending on the type of contraception a person is using. People may notice their symptoms get better after they change birth control.
Estimates for how common PMS is vary.
The Office of Women’s Health explain that
A
According to the American College of Obstetricians and Gynecologists, a healthcare provider will make a clinical diagnosis of PMS when:
- symptoms interfere with daily activities
- symptoms appear 5 days before the period starts and end 4 days within it starting
- symptoms occur for at least 2–3 months
A smaller number of people experience a severe form of PMS called PMDD.
Treatment options for PMS vary depending on a person’s specific symptoms.
People can manage PMS symptoms by taking medications, making dietary changes, exercising, trying self-care methods, and making other lifestyle changes.
Medication
Taking OTC and prescription medication can help relieve painful symptoms, such as abdominal cramps and headaches.
Examples of medication that people take to treat PMS include:
- pain relievers such as acetaminophen, which can help relieve muscle pain, cramps, and headaches
- nonsteroidal anti-inflammatory drugs, which can reduce cramp pain, headaches, and muscle aches
- diuretics, which can help relieve bloating and breast soreness
For severe PMS symptoms, a doctor may recommend that a person starts taking hormonal birth control pills to reduce PMS symptoms. These drugs work by affecting the levels of estrogen and progesterone in the body.
Speak to a doctor about severe PMS. They may prescribe medications to relieve depression, anxiety, or other mood-related symptoms.
Use relaxation techniques
Managing stress and using relaxation techniques, such as deep breathing or meditation, can help regulate emotional imbalances due to PMS.
Other examples of stress management and relaxation techniques include:
- yoga
- tai chi
- stretching
- taking a bath
- going for a walk
- journaling
- speaking with a close friend or loved one
- meeting with a mental health counselor or therapist
Try gentle exercise
Exercising gently can increase estrogen and progesterone levels, which may help reduce PMS symptoms.
A
- nausea
- constipation or diarrhea
- swelling of breasts
- bloating
- flushing
- increased appetite
It is worth noting that uncontrolled external factors, such as sleep patterns, nutrition, and the participants’ living environments, could have affected these results.
In contrast, the results of a
Relieve bloating
Bloating can make a person feel heavy and lethargic. People can reduce PMS-related bloating by:
- not eating salty foods, which make bloating worse
- eating potassium-rich foods, such as bananas
- staying hydrated
- doing gentle exercise
Learn more about how to relieve menstrual bloating here.
Relieve menstrual cramps
Menstrual cramps usually arise a few days before the period starts and can last for several days. Trying home remedies such as applying heat to the abdomen, doing gentle exercise, trying massage, and using essential oils can help.
Learn more about how to relieve menstrual cramps here.
Eat certain nutrients
Making some dietary changes may reduce mild to moderate PMS symptoms. The following are some examples of nutrients that may help a person manage their PMS symptoms:
- Magnesium may help relieve migraine episodes related to PMS. Leafy green vegetables, such as kale and spinach, contain magnesium.
- Fatty acids may help reduce abdominal cramps related to PMS. Good sources include fish, nuts, and green vegetables.
- Calcium supports bone strength and density. Having adequate calcium levels also helps regulate mood, sleep, and food cravings.
A 2017 double-blind trial study reported that college-age females who consumed 500 milligrams of calcium daily for 2 months had significant reductions in depression, anxiety, and water retention related to PMS.
Most females experience at least one symptom of PMS. Fluctuations in hormone levels might play a significant role in PMS, but the exact cause remains unknown.
A small percentage of people can develop a severe form of PMS called PMDD.
Taking OTC pain relievers, making appropriate dietary changes, and managing stress may all help reduce PMS symptoms.
People may wish to see their doctor if symptoms do not improve, if they worsen despite treatment, or if they interfere with their ability to perform daily tasks.
