Psoriatic arthritis can develop in people who have psoriasis, and it affects many joints, including the knee.
Psoriasis is a skin condition that causes skin cells to build up and form patches of itchy, dry skin called plaques.
If a person with psoriasis develops psoriatic arthritis as well, it may cause one or more joints, such as the knee, to become stiff, inflamed, and painful.
Psoriatic arthritis is a long-term inflammatory disease. Symptoms may get progressively worse over time without effective treatment.
It is possible, however, to slow the progress of the condition with the correct treatment. Early diagnosis is vital to minimize damage to the joints.
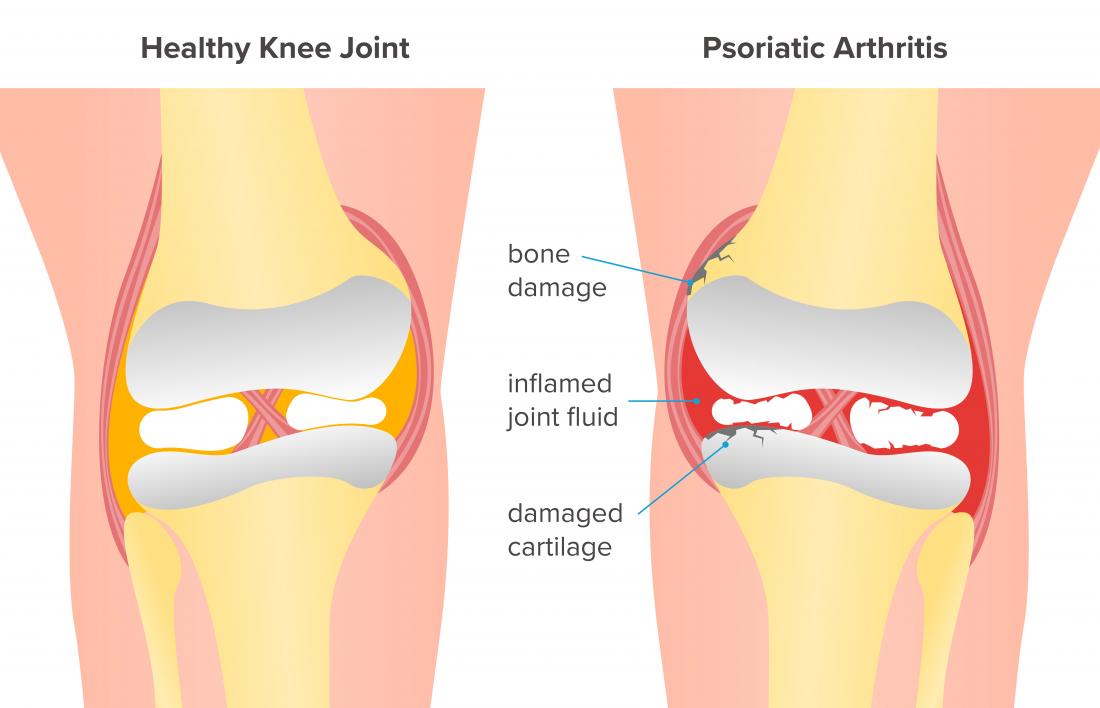
Image credit: Stephen Kelly, 2018.
Psoriatic arthritis does not follow the same pattern in everyone. The symptoms, such as stiffness and painful swelling, may appear differently in each person.
For example, some people with psoriatic arthritis of the knee will experience symptoms in one knee, while others will experience symptoms in both knees.
Psoriatic arthritis in the knee may also cause swelling in the ligaments, tendons, and synovial fluid in the surrounding area. Symptoms may also show up in the elbows, feet, and hands.
Some people may notice slight stiffness or pain in just one of their knees, whereas others may have severe pain in both knees that makes it difficult to walk.
Symptoms of psoriatic arthritis in the knee may vary from person to person. Common symptoms include:
- stiffness, especially after resting or sleeping
- swelling and inflammation in the knee and surrounding area
- pain in the joint, tendons, or ligaments
- feeling that the joint is stuck, difficult to move, or has a reduced range of motion
- warm or hot skin on the knee due to inflammation
A person may also experience other symptoms not confined to the knee, including:
Symptoms may go through a pattern of relapses and remissions. A person may have a sudden attack where symptoms get worse over a short time.
After the flare-up, symptoms may improve as the condition goes into remission. The symptoms may stay away for a long time until the next flare-up.
The severity of a person’s psoriasis symptoms does not always determine that of their psoriatic arthritis symptoms. For instance, a person may have severe psoriasis symptoms but only mild psoriatic arthritis symptoms.
Likewise, someone with only mild psoriasis may still experience more severe psoriatic arthritis.
Psoriatic arthritis occurs because the body’s immune system mistakenly attacks healthy cells and tissues.
In people with psoriasis, the faulty immune response causes the body to make new skin cells very quickly, which stack on top of each other and form plaques.
When the condition affects the joints, it leads to inflammation.
While there is no clear cause for psoriatic arthritis,
People whose close relatives have psoriatic arthritis may be more likely to also develop the condition.
A 2017 review that appears in The New England Journal of Medicine also noted other factors that may influence the development of psoriatic arthritis, such as:
- obesity
- severe psoriasis
- nail disease
- traumatic injuries
- smoking
The condition may occur at any age, but according to the National Psoriasis Foundation, most people with psoriatic arthritis first notice symptoms about 10 years after their psoriasis begins. Symptoms often begin between the ages of 30 and 50.
Not all people with psoriasis develop psoriatic arthritis. In fact, psoriatic arthritis only occurs in about 30 percent of people who have psoriasis.
Doctors can use imaging tools to help them diagnose psoriatic arthritis in the knee. Using MRI, X-rays, or an ultrasound of the knee may help them check for irregularities or signs of inflammation in the joint and surrounding tissues.
Doctors can use additional tests to rule out other common forms of arthritis, such as rheumatoid arthritis and osteoarthritis.
They may also order blood tests to check for inflammation and specific antibodies from other types of arthritis.
In some cases, they may remove some fluid from the joint to help eliminate the possibility of other underlying conditions, such as infections.
There is currently no cure for psoriatic arthritis, but emerging treatments are showing promise for long-term management of the condition. Other treatments focus on managing symptoms and increasing the quality of life.
Biologics
Current
These drugs can help block TNF, which plays a key role in inflammation. They are proving effective at reducing the severity of symptoms and the frequency of flares.
However, biologics can cause unwanted side effects, especially in people who experience frequent infections. Anyone who uses biologic therapy will need routine monitoring for these effects.
A doctor will explain more about biologics and describe other options.
Oral small molecule drugs
If a person cannot use biologic therapy, the doctor may recommend another new class of drugs called oral small molecules (OSMs). Examples include apremilast (Otezla) and tofacitinib (Xeljanz).
Disease-modifying antirheumatic drugs
Like biologics and OSMs, disease-modifying antirheumatic drugs (DMARDs) are a long-term option. They may slow the progression of psoriatic arthritis. Examples include methotrexate and cyclosporine.
DMARDs work best when a person starts taking them as early as possible in the disease progression.
They can take time to work, so it is important to continue taking them, even if symptoms do not improve immediately.
Treating symptoms
Doctors may prescribe nonsteroidal anti-inflammatory drugs (NSAIDs) and corticosteroid injections when symptoms flare in the knee.
These are short-term treatments that aim to provide immediate relief. Long-term use can lead to side effects.
Many people may find some relief from psoriatic arthritis in their knees using home remedies, including:
- taking over-the-counter NSAIDs such as ibuprofen (Advil) or naproxen (Aleve)
- alternating applying ice and heat packs
- gently exercising to promote range of motion
- gently stretching or taking yoga classes to help relax tight muscles
Some additional alternative therapies may be helpful to manage pain, but they may not work in everyone. These include acupuncture, massage, an anti-inflammatory diet, and electrical stimulation.
Doctors may also recommend that the person maintains a healthy weight through exercise and diet to reduce pressure and stress on their joints.
In some cases, wearing special shoes may help reduce symptoms in the feet and knees.
Psoriatic arthritis of the knee is a chronic condition. Successful treatment involves working closely with a healthcare provider to discuss any medications and their side effects to find a treatment for the pain and help stall the condition’s progression.
Pain and inflammation from psoriatic arthritis in the knee can disrupt a person’s everyday life. While there is currently no cure for psoriatic arthritis, there are many medications and home remedies available to help manage symptoms and reduce pain.
